How to Analyse a Skeleton for Signs of Trauma

Share this step
Analysing a skeleton for signs of trauma is an important component of forensic practice. The presence of healed fractures (ante-mortem) can be useful for establishing an individual’s identity through comparison with medical records. The presence of fractures that occurred around the time of death (peri-mortem) may be useful for establishing the circumstances of death, or trauma consistent with the cause of death. It is important to identify breakage or damage which has occurred to the skeleton after death (post-mortem), so that peri-mortem fractures are not overlooked or misidentified.
Fractures
Bones in living people have a certain degree of elasticity in response to forces applied to them, which essentially means that they can bend slightly before returning to their normal shape. When forces applied to bone are greater than the elastic potential, it can result in ‘plastic deformation’ to the bone, which is a permanent alteration. This is sometimes seen on the skulls of people who have a slight depression that has occurred in response to trauma. If the force applied is greater than this, the structure of the bone can fail and a fracture occur.
After a bone has fractured, bleeding occurs at the fracture edges. After approximately one-week, woven bone may just be visible at the site of the fracture. This develops into a fracture callus which gradually hardens as the bone heals. The callus will remodel over time, but the site of the fracture is usually still visible many years afterwards and there is often a slight deformity caused by angulation or overlap of the fractured ends as they heal.
Ante-mortem, peri-mortem and post-mortem trauma all have different features, which help to distinguish them. The features of each are described below.
Ante-mortem trauma
Ante-mortem trauma is useful for establishing an individual’s identity because it can be matched to medical records or personal knowledge of the deceased. Injuries can be identified as ante-mortem if they show signs of healing, either partial or complete. After one to two weeks, signs of healing will be visible at the fracture edge. Some key features of ante-mortem trauma are:
- Injuries show some signs of healing, either partial or complete.
- If the fracture is well-healed, it is difficult to establish how much time has elapsed since the fracture occurred.
- Different people will heal at different rates depending on a range of factors, including the age of the person, their health status, and whether the fracture edges have been effectively reduced and immobilised.
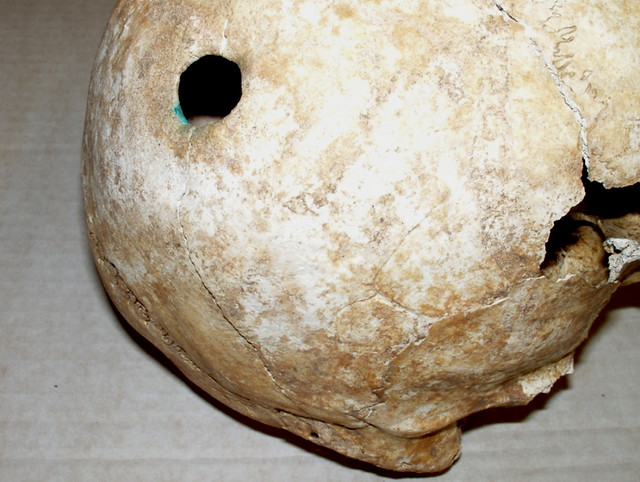 Ante-mortem healed trepanation to the skull. Note the edges are rounded indicating healing. The green stain is due to a copper alloy object being placed over the hole
Ante-mortem healed trepanation to the skull. Note the edges are rounded indicating healing. The green stain is due to a copper alloy object being placed over the hole
 Ante-mortem fracture to the shaft of the femur. The bone had been broken in two places and it has healed in a slightly angulated manner that would have been visible in the person’s leg and have affected their gait.
Ante-mortem fracture to the shaft of the femur. The bone had been broken in two places and it has healed in a slightly angulated manner that would have been visible in the person’s leg and have affected their gait.
Peri-mortem trauma
Evidence of peri-mortem trauma can provide important information about the circumstances surrounding death, or even the cause of death. As a result, peri-mortem injury will show no signs of healing. The term ‘peri-mortem’ when applied to skeletons, is not quite the same as in a clinical setting where soft tissues can also be observed. This is because the time resolution is not as clear-cut as it is with soft tissue. When looking only at the skeleton, peri-mortem basically refers to trauma to ‘fresh bones’. Some key features of peri-mortem trauma are:
- Injuries show no signs of healing.
- Injuries could reveal the cause of death, or even be associated with attempts to conceal the deceased’s body (e.g. dismemberment).
- The characteristics of the fracture could indicate whether a weapon was used to cause death and the type of weapon (e.g. gunshot, or knife type).
- Examination of the location of wounds is also significant as this can suggest a positional relationship between attacker and victim, as well as whether the injury was self-inflicted or inflicted by another party.
 An example of peri-mortem trauma to the skull inflicted with a sharp-edged weapon
An example of peri-mortem trauma to the skull inflicted with a sharp-edged weapon
The distinction between peri-mortem and post-mortem for forensic anthropologists is really more of a differentiation between damage done to ‘dry’ bone rather than ‘fresh’. There are a number of morphological characteristics that can help differentiate peri-mortem from post-mortem trauma. Living bone that is surrounded by soft tissues breaks differently to ‘dry’ bone. Linda Fibiger (2014) highlighted key features of peri-mortem trauma as follows:
- Depressed but adhering bone
- Oblique angles on fracture margins
- Smooth edges to fracture margins
- Secondary linear and concentric radiating fractures
- Contrecoup fractures
- Bevelling or flaking on the inner aspects of the primary defect
- Consistent colouring between the fracture surface and adjacent bone
 This skull has peri-mortem trauma, as identified by the consistent colouring, smooth fracture edges and lack of healing.
This skull has peri-mortem trauma, as identified by the consistent colouring, smooth fracture edges and lack of healing.
 Hip bone with a penetrating injury. Note the adhering flakes of bone
Hip bone with a penetrating injury. Note the adhering flakes of bone
Post-mortem trauma
Post-mortem trauma includes any form of damage to the bone after death. The bones of the skeleton often become fragmented by mechanical forces operating on the body in the ground. When bone decays, the soft tissues decompose and the bones become ‘dry’. Dry bone has limited moisture and collagen compared to fresh bone and therefore has less elasticity. The fracture edges in ‘dry’ bone have different characteristics to the fractures in ‘fresh’ bone. In dry bone the edges are often:
- Lighter in colour than the surrounding bone.
- At right angles to the bone and more jagged in appearance and there will be no adhering bone fragments.
- There will also be no radiating or concentric fracture lines.
 This skull shows a clean, circular hole in the top of the head. The white colouration and clean, sharp edges indicate that this is post-mortem damage.
This skull shows a clean, circular hole in the top of the head. The white colouration and clean, sharp edges indicate that this is post-mortem damage.
Assessing Trauma
To assess trauma in a skeleton, it can be useful to pose a series of questions, focusing your analysis. Some good examples are as follows:
- Are there any signs of trauma on the skeleton?
- Is the trauma ante-mortem, peri-mortem or post-mortem?
- If it is ante-mortem, is it healed or not?
- Can the injury be associated with medical records to establish identity?
- Was the trauma likely caused by accidental or intentional violence?
- Was the trauma caused by blunt force or sharp force trauma?
- Is the trauma peri-mortem and if so is it consistent with the cause of death?
Have you suffered from a fractured bone that has affected the way that you live or get around? Did the bone take longer to heal than expected?
As you’ve just learned, trauma can be ante-, peri-, or post-mortem. It can also be further categorised based on the type of weapon or force used to inflict the injury.
Share this

Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free








