Community health workers: who are they and what do they do?

Share this step
At the heart of the community health system is the community health worker.
Who do you think of as community health workers?
- The village midwife who delivers babies in the home
- The community educator who provides health education messages
- The volunteer who accompanies patients to the nearest health facility
- The trained villager who provides first aid and advice in emergencies
Community health workers come in many different sizes and shapes, but we can identify some common characteristics.
A community health worker or CHW:
- Is based in the community rather than a formal health facility
- Provides support and assistance to communities in preventive health measures, and may provide some basic curative care and assistance in accessing formal health services
- May be paid or a volunteer
- Is not a health professional, but has received some basic training, and has some linkage to the formal health service.
Why is the CHW important?
The CHW provides a bridge between formal providers of health or social services, and the communities they serve.
What do CHWs do?
CHWs can deliver a range of preventive, promotive and curative health services and can contribute to reducing inequities in access to care. These include maternal, newborn and child health; communicable disease control; mental health services; sexual and reproductive health care; and non-communicable disease prevention and control.
CHWs are uniquely positioned to support communities to address their own health needs, as well as motivating community participation and ownership.
Can you think of an example of a community health worker that you have encountered?
Although CHWs are widely used in health services, their effectiveness varies considerably.
Some of the key factors that influence the effectiveness of CHW include:
- The extent of support and relationship with the local public health services, and thus sense of accountability towards the system amongst CHWs;
- The level of credibility, legitimacy and assurance (of being part of the local public health services) amongst CHWs and the community they serve.
- The social status and welfare of the CHWs in terms of the incentives or opportunities to earn sufficient remuneration for their own livelihood.
The guidelines emphasise three key areas for the management and operation of CHW programs:
(a) Selection, training and certification of CHWs. Important factors include ensuring community membership and acceptance, training based on expected roles and responsibilities, and use of appropriate practice focused training methods;
(b) Management and supervision of CHWs. Here factors include supportive supervision, appropriate remuneration or incentives, clear agreement on roles and responsibilities, and establishment of career progression.
(c) Integration into the formal health system and local communities. Factors identified here include ensuring the provision of adequate commodities and consumables for CHW usage; and involvement of the communities in selection of CHWs and in provision of resources to support local community health activities.
The role of CHWs as links between communities and formal health services is central to effectiveness. While some CHWs work closely with health facilities and others independently, the bridging activities of CHWs between communities and health services in the form of referral and feedback links provide increased opportunities for the successful preventative and curative services, as well as a mechanism for establishing the community as managers and owners of local health initiatives.
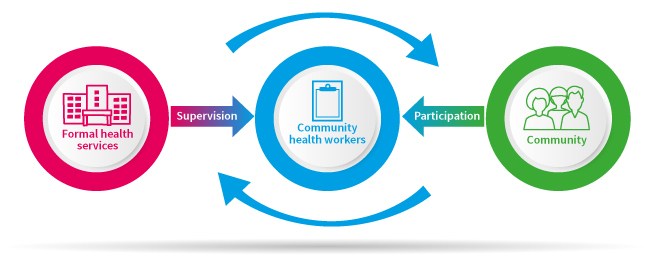
Successful programs are also dependent on formal health staff creating a supportive environment for CHWs. Many health staff have no experience or training in how to develop constructive relationships with CHWs, and are generally not engaged in the planning, implementation, or monitoring of CHW programs. This can lead to poor attitudes towards CHWs by health staff.
Community participation in community-level health systems is crucial for successful community health service programs. While it is difficult to define what community participation means for different contexts, communities need to be involved in different parts of the program to maintain ownership and active participation, which are preconditions for sustainability and impact. This includes participation in the selection of CHWs, identifying health needs and priorities, involving them in all aspects of the program, such as in planning and monitoring, providing support to CHWs through monetary and/or non-monetary incentives, and supervising CHWs, given that CHWs should be answerable and accountable to the community in which they work.
There has been much debate about whether CHWs should be paid or voluntary. Evidence shows that volunteerism is usually not sustainable long term. Monetary incentives can increase retention. But these can also be problematic when there is inequity in incentives among different types of community workers or when incentives are inconsistent. Non-monetary incentives are important, particularly in the form of community recognition and respect, the acquisition of skills, and personal growth and development.
While CHW programs and community health service packages can make a valuable contribution to primary health care, CHW programs do require considerable investment in terms of training, support, supervision, and task allocation. CHW programs should not be perceived as a remedy for weak health systems and (while cost-effective) they are not a cheap alternative to formal health services if proper remuneration, training and supervision are provided.
Do you think CHWs should be paid or voluntary? Look up the recommendations from the World Health Organization on page 47 of the WHO guideline on health policy and system support to optimize community health worker programmes report available in the ‘see also’ section below.
Do you agree with the WHO recommendations? If so why? Or if not, why?
Please comment below.
References
Kane, SS, Gerretsen, B, Scherpbier, R, Dal Poz, M, and Dieleman, M, 2010, ‘A realist synthesis of randomised control trials involving use of community health workers for delivering child health interventions in low and middle income countries’, BMC health services research, vol. 10, no. 1, p.286.
World Health Organization, 2018. WHO guideline on health policy and system support to optimize community health worker programmes. World Health Organization, viewed 26 June, 2019, <https://apps.who.int/iris/bitstream/handle/10665/275474/9789241550369-eng.pdf>.
Share this

Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free








