The Vital Statistics of COVID-19
Share this step
COVID-19 is a new pathogen and almost everything known about it has been discovered since December 2019. Great uncertainty remains about its characteristics.
What is SARS-CoV-2? What is COVID-19?
Severe Acute Respiratory Syndrome Coronavirus-2, (SARS-CoV-2), is the name given to the 2019 novel coronavirus. COVID-19 is the name given to the disease associated with the virus. SARS-CoV-2 is a new strain of coronavirus that has not been previously identified in humans. [1]
This section lists the main things known about the pathogen and will be used as a reference throughout the course.
Symptoms
The symptoms of COVID-19 are non-specific and the disease presentation can range from no symptoms (asymptomatic) to severe pneumonia and death. Symptoms include:
| fever | 87.9% |
| dry cough | 67.7% |
| fatigue | 38.1% |
| sputum production | 33.4% |
| shortness of breath | 18.6% |
| sore throat | 13.9% |
| headache | 13.6% |
| myalgia or arthralgia | 14.8% |
| chills | 11.4% |
| nausea or vomiting | 5.0% |
| nasal congestion | 4.8% |
| diarrhoea | 3.7% |
| anosmia (loss of smell) [4] | 30% |
Source: [2, pages 11-12]
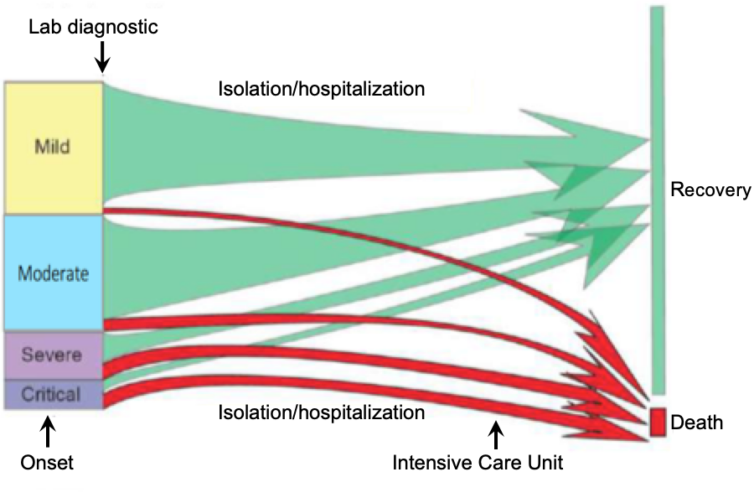
Most people infected with COVID-19 virus have mild disease and recover.
Approximately 80% of laboratory confirmed patients have had mild to moderate disease, which includes non-pneumonia and pneumonia cases, 13.8% have severe disease (dyspnea, respiratory frequency ≥ 30/minute, blood oxygen saturation ≤ 93%, PaO2/FiO2 ratio < 300, and/or lung infiltrates > 50% of the lung field within 24-48 hours) and 6.1% are critical (respiratory failure, septic shock, and/or multiple organ dysfunction/failure).
Asymptomatic infection has been reported, but the majority of the relatively rare cases who are asymptomatic on the date of identification/report went on to develop disease. The proportion of truly asymptomatic infections is unclear but appears to be relatively rare and does not appear to be a major driver of transmission. [But see below]
Individuals at highest risk for severe disease and death include people aged over 60 years and those with underlying conditions such as hypertension, diabetes, cardiovascular disease, chronic respiratory disease and cancer.
Disease in children appears to be relatively rare and mild with approximately 2.4% of the total reported cases reported amongst individuals aged under 19 years. A very small proportion of those aged under 19 years have developed severe (2.5%) or critical disease (0.2%).
Mortality increases with age, with the highest mortality among people over 80 years of age (Crude Fatality Ratio 21.9%).
The CFR is higher among males compared to females (4.7% vs. 2.8%).
By occupation, retirees had the highest CFR at 8.9%.
Patients who reported no comorbid conditions had a CFR of 1.4%,
Patients with comorbid conditions had a much higher CFR: 13.2% for those with cardiovascular disease, 9.2% for diabetes, 8.4% for hypertension, 8.0% for chronic respiratory disease, and 7.6% for cancer. [1, page 12]
In South Korea, where testing has been more widespread, 30% of patients testing positive have had anosmia (loss of smell) as their major presenting symptom in otherwise mild cases. [4]
People with COVID-19 generally develop signs and symptoms, including mild respiratory symptoms and fever, on an average of 5-6 days after infection (mean incubation period 5-6 days, range 1-14 days).[2]
Using available preliminary data, the median time from onset to clinical recovery for mild cases is approximately 2 weeks and is 3-6 weeks for patients with severe or critical disease. Preliminary data suggests that the time period from onset to the development of severe disease, including hypoxia [a condition in which the body or a region of the body is deprived of adequate oxygen supply at the tissue level], is 1 week. Among patients who have died, the time from symptom onset to outcome ranges from 2-8 weeks. [2]
Last week, scientists in Germany reported that people infected with COVID-19 seem to be most contagious in the first week of showing symptoms. During this time they found very high levels of viral shedding – where the virus leaves a cell to either infect other cells in the body, or those in other people – especially in the throat and lungs. The researchers also found that after 10 or 11 days of first showing symptoms people continued to have the virus in their sputum, but in low enough levels that they could be discharged from medical care.
As the amount of virus in the body steadily reduces over the course of infection, the question remains how long infected people stay contagious. It’s a critical aspect still being studied, since the presence of the virus doesn’t necessarily mean they are able to infect other people.
A study conducted in two hospitals in Wuhan, China, in March this year showed that the virus was on average still being shed by cells in the human body 20 days after infection, and in some patients even after 37 days. [3]
COVID-19: What proportion are asymptomatic?
Everywhere we look we cannot get a handle on the essential facts or at times we get 2 completely different answers to the same question. So, we thought we would try to answer an important question: what is the proportion of people with SARS-COV-2 who are asymptomatic? To answer this we searched LitCovid (a subset of Pubmed), medRxiv, Trip, Scholar and Google. We retrieved 21 reports for analysis. What did we learn:
That between 5% and 80% of people testing positive for SARS-CoV-2 may be asymptomatic
That symptom-based screening will miss cases, perhaps a lot of them That some asymptomatic cases will become symptomatic over the next week (sometimes known as “pre-symptomatics”)
That children and young adults can be asymptomatic
We also learnt that there is not a single reliable study to determine the number of asymptotics. It is likely we will only learn the true extent once population based antibody testing is undertaken. [7]
Summary
- the main symptoms of COVID-19 include fever, a dry cough, fatigue and loss of smell.
- approximately 80% have mild to moderate disease
- approximately 14% have severe disease and 6% are critical
- most at risk are ≥ 60 and above, and those with underlying conditions
- mortality is highest in the over-80s with Crude Fatality Ratio 21.9%
- disease is rare and mild in people under 19 years (2.5% severe/critical)
- CFR is highest in males (4.7%) compared to females (2.8%)
- retirees have the highest CFR at 8.9%
- the mean incubation time for COVID-19 is 5.2 days in a range of 14 days
- COVID-19 is most contagious in the first week after showing symptoms
- the basic reproduction rate for COVID-19 is estimated at 1.4 to 5.6
- the median time from onset to recovery for mild cases is about 2 weeks
- the median recovery time is 3-6 weeks for severe or critical cases.
References
[1] ECDC, “Q & A on COVID-19”, European Centre for Disease Prevention and Control, 1 March 2020, Viewed 22nd May 2020. https://www.ecdc.europa.eu/en/covid-19/questions-answers
[2] Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19), 16-24 February 2020
[3] Gavi, ‘When is COVID-19 most contagious and why is self-isolation so important?’ 6 April 2020 https://www.gavi.org/vaccineswork/when-covid-19-most-contagious-and-why-self-isolation-so-important
Extra References Added During the Presentation
[4] Claire Hopkins, Nirmal Kumar, ‘Loss of sense of smell as marker of COVID-19 infection’, ENT UK, undated – probably April 2010. Link to article
[5] Graham Lawton, ‘Why are men more likely to get worse symptoms and die from covid-19?’, New Scientist, 16 April 2020 https://www.newscientist.com/article/2240898-why-are-men-more-likely-to-get-worse-symptoms-and-die-from-covid-19/
[6] By Danny Hakim, ‘Asthma Is Absent Among Top Covid-19 Risk Factors, Early Data Shows’. The New York Times,Published April 16, 2020, Updated April 20, 2020 https://www.nytimes.com/2020/04/16/health/coronavirus-asthma-risk.html?referringSource=articleShare
[7] Carl Heneghan, Jon Brassey, Tom Jefferson, ‘COVID-19: What proportion are asymptomatic?, Centre for Evidence-Based Medicine, Oxford University, April 6, 2020 https://www.cebm.net/covid-19/covid-19-what-proportion-are-asymptomatic/
[8] gov.uk, ‘Statement from the UK Chief Medical Officers on an update to coronavirus symptoms: 18 May 2020. New information about coronavirus (COVID-19) symptoms has been announced.’ 18 May 2020, Department of Health and Social Care https://www.gov.uk/government/news/statement-from-the-uk-chief-medical-officers-on-an-update-to-coronavirus-symptoms-18-march-2020
Share this
COVID-19: Pandemics, Modelling, and Policy

Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free







