Retinopathy of Prematurity (ROP): Parental Involvement
Share this step
Adapted from ‘Involving the parents of preterm babies.’ Comm Eye Health Vol. 30 No. 99 2017 pp 60-61 and an interview with the mother of a preterm baby in the United Kingdom.
Screening for retinopathy of prematurity (ROP) starts in the neonatal unit but can continue even after babies have been sent home with their parents. Parents need to understand the importance of both screening and its timing so they will bring their baby back at the right time.
Parents also need to know that laser treatment, if needed, cannot be delayed and that their child will need regular follow up visits afterwards to ensure treatment was successful in the short term and to detect and manage any complications in the long term.
Case study: A mother’s perspective of ROP screening
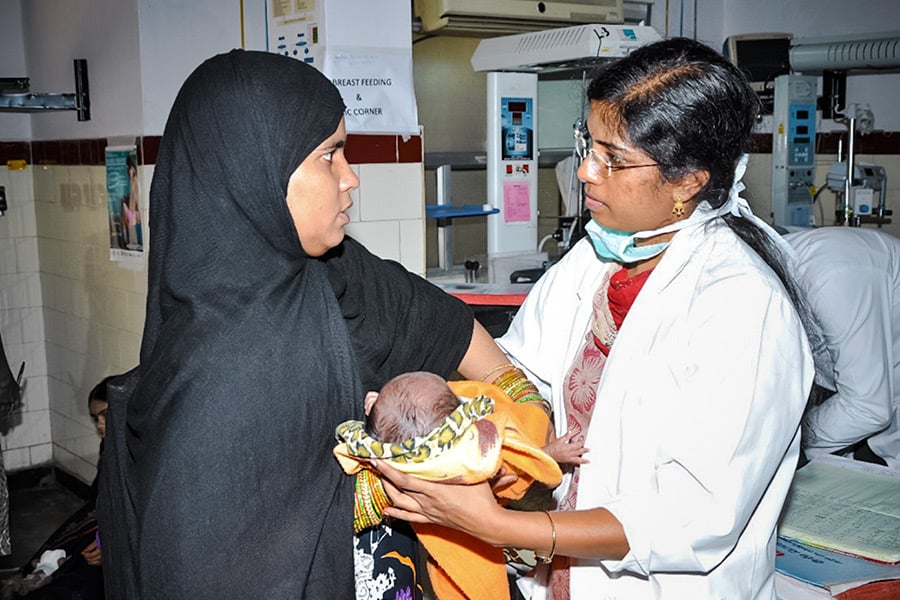
Active engagement of the parents can make all the difference between success and failure in preserving a child’s vision.Liz (mum) experienced light bleeding at 23 weeks pregnancy and, despite all the best efforts of the hospital, her daughter Josie was born 24 weeks premature. Josie spent more than 137 days in the neonatal intensive care unit (NICU) due to multiple health concerns. Liz recounts her experience with ROP in parallel to the other needs of her baby which meant they went from one level of hospital to another.Liz: ‘We were first told about ROP at Bolton (the first hospital) in the first week Josie was born. The nurses touched on it verbally but with her being so small we were worried about her thriving and didn’t ask too much detail. When Josie was 1 week old (chronological age) we transferred to a hospital in Manchester. During the ROP screening, it was Julie (the neonatal ROP nurse) who came to talk to us and told us more about ROP. Due to the vessels looking “angry” they did weekly checks, when it reached stage three ROP, they carried out injections. I was panicking. I kept thinking she was going to go blind. I was an emotional wreck and crying at everything. Julie just sat me down and explained that Josie needed treatment, that they’ve caught it early and she will have some vision loss, like short vision. She has regular check ups and recently had to have laser treatment and still has follow up checks’Liz holding Josie for the first time, a very special moment for them both © Liz Dootson CC-BY-NC-SA-4.0
‘The nurse also gave us written information and showed us the internet website Bliss, which I read and find very helpful. One of the nurses gave us a leaflet and she used a diagram of the eye to explain what stage of ROP Josie had. She broke it down into the quadrants in the eye and then gave us another leaflet about the treatment. I was told mainly by the bedside about Josie and what treatment she needed which I think could have been done differently as you’ve got other parents around and they are listening in.’
Supporting communication with parents and caregivers
-
What is ROP and why does it occur?
-
How common is ROP?
-
How is ROP detected?
-
What should we expect during and after an eye examination? Images of the normal retina and the retina with ROP can be a very useful way to educate parents about ROP.
-
Will my child need treatment?
-
What happens if my baby is unwell?
-
Where can I find out more? Provide website addresses if appropriate.
-
Contact details for members of the neonatal team or the ophthalmologist.

Click to expand
Inside of a printed ROP booklet for parents
© Indian Institute for Public Health CC BY-NC-SA 3.0
Systems to support parental involvement
Liz: ‘Before the treatment, I just went into a separate room with the eye doctor, and Josie’s nurse. And he went through everything, the treatment outcomes and follow-up. I then had to signed a consent form. So that was all done really well. The nurse was there for the treatment with a ventilator to support Josie even after the laser. I trusted her with Josie.’
-
The appointment date, time and place, this may be in the unit or in the hospital where the ophthalmologist works
-
Who to contact if there are problems
-
Details about transport assistance or reimbursement of costs for travel, if appropriate
-
Information about the consequences of late screening and the potential risk of blindness if screening does not take place.
Liz: ‘I cry about everything and still do. She was having weekly checks, her eyes are doing really well. They went to every two weeks, but these last couple of eye checks, they have noticed that some of the vessels have started to grow a little bit, they call it suspicious. I do feel like he will do some more laser treatment shortly. And Julie (the ROP nurse) is always around. She always makes sure that we’ve understood what the eye doctor has said. She also explains things if we have not understood it.’‘We’ve got the appointment time and if we feel like we can’t make them, we can make them slightly later. I have a diary which helps to organise appointments for vaccinations and all checkups, including ROP. Sometimes I ring Julie just to confirm appointments and they send text messages as well.’‘So there was one other family we got quite friendly with and their daughter was having ROP. So we have gone through quite a lot of similar things. So it was nice to be able to talk to her about it.’‘Follow-up is important because, if she didn’t have the ROP check or treatment, ROP can blind babies.’
Conclusion
Good communication is an art which can be improved. It supports parental involvement which in turn contributes to good medical care and better outcomes for a baby with ROP. Supporting parents along the way is a long term commitment for all ROP programmes.
Reflecting on the case study, what were the most striking elements for you of Liz’s experience of ROP screening and treatment?
What resources need to be available to support parents with preterm babies? How are follow-up checks taking place during the COVID-19 pandemic in your setting?
Share this
Retinopathy of Prematurity: Practical Approaches to Prevent Blindness

Retinopathy of Prematurity: Practical Approaches to Prevent Blindness


Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free







