Example of applied implementation science

Share this step
Now that you have been given the introduction to implementation science, we are going to use a real example of existing research which is using implementation science from the outset to develop contextually fit solutions to the problem of optimising antibiotic use in surgical pathways.
We are going to refer back to the ASPIRES study which was introduced to you in week two.
The main research question that the ASPIRES study is trying to address is: How can antibiotic use be optimised along the entire surgical pathway – that is before, during and after surgery and in the different settings (home, primary and hospital care)? This involves developing behavioural, structural and technological interventions which are context specific.
The research involves a multidisciplinary team looking at this issue in England, Scotland, South Africa, India and Rwanda, and involves:
- in-depth examination of the surgical pathway context (healthcare organisation, home, and national level policies and constraints) using strategic analysis and ethnography
- co-design and implementation of interventions
- evaluation (health outcomes and economic) using a ‘system dynamics’ approach which models the impacts of parallel interventions, and how they conflict or help towards the intended aim
Overarching theoretical approaches
This project offers a comprehensive investigation of Antimicrobial Stewardship (AS) and Infection Control (IC) behaviours approached as a co-construction of individual, organisational and wider contextual factors. The project examines these factors at the micro-, meso- and macro-levels using theoretical approaches from the fields of strategic management, sociology, psychology, and anthropology. To evaluate how appropriate interventions may be successfully adopted and implemented within different contexts, an organising framework of implementation is employed.
A soft systems approach is used for the evaluation of different interventions and policies by mapping interactions and consequences using qualitative and quantitative data. To connect these multi-level and multidisciplinary approaches, the Consolidated Framework for Implementation Research (CFIR) is used as an overarching organising framework as it facilitates understanding of processes of introduction and management of change within a complex healthcare system or pathway and allows for examination of behaviours.
WP1 – Health System level factors: PESTELI framework
Methods
To provide an assessment of the ‘outer’ context, a framework from the disciplines of strategic and health management has been adapted and employed; PESTELI: Political factors, Economic influences, Sociological trends, Technological innovations, Ecological factors, Legislative requirements, Industry analysis. Analysis from the perspectives of key stakeholder groups at the macro-national level and at the meso-organisational level is included.
Secondary data
Textual sources including policy documents, guidelines, board minutes, reports and strategies; structural process and outcome performance indicators.
Primary data
Key informant interviews including professional organisations, professionals, and public/patient advocacy groups.
WP2 – Roles and context: Ethnographic research
Methods
Ethnographic research involving direct observation of practice along the entire surgical pathway and interviews with stakeholders involved in the pathway will be conducted. This research will draw on the symbolic interactionist research tradition by understanding the division of labour as emerging through social interaction. Data collection will span four months in each country. Direct observations will take place in pre-, intra-, and post-operative settings in outpatient clinics, operating theatres and surgical wards. Drawing on a definition of culture in Figure 1 to study antibiotic decision-making in surgical teams.
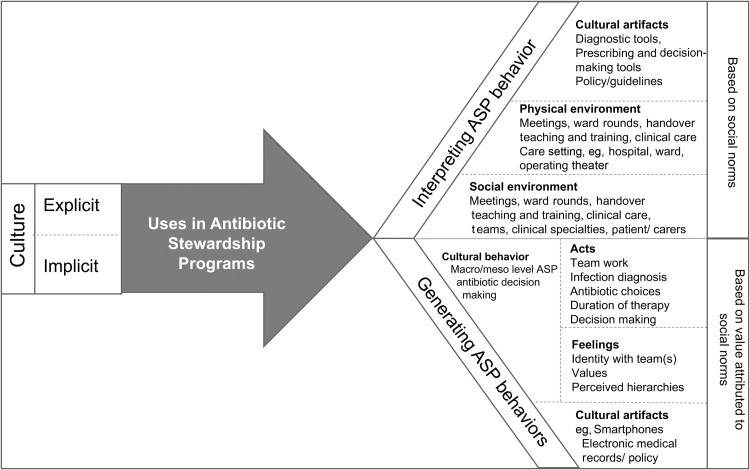
Figure 1 – 1 Charani et al., Clinical Infectious Diseases 2019 Jun 18;69(1):12-20. d
WP3 – Intervention design and implementation: Consolidated Framework for Implementation Research (CFIR) analysis
Methods
Scoping literature review for interventions implemented and/or evaluated. Outputs from WP1 & WP2 will provide a comprehensive assessment of the ‘outer’ and ‘inner’ contexts, including existing interventions in the study sites. For any new interventions, co-design workshops will provide an assessment of contextual fit. Pilot implementation will be carried out over a six-month period: providing proof of concept data and variables for WP4.

Figure 2 – Multidisciplinary workshops to co-develop antimicrobial stewardship interventions in surgical pathways, Kerala India Photo Credit Dr Sanjeev Singh Amrita Institute of Medical Sciences
WP4 – Operational and economic evaluation: System Dynamics
Methods
The full System Dynamics (SD) methodology cycle. Starting with boundary setting, problem structuring and then capturing influence factors and ‘feedback loops’ when multiple interventions are implemented concurrently; this WP4 will employ data gathered in WP1-3 and use stakeholder workshops to validate the emergent model in England and India. The system/unit of analysis will be defined iteratively from ward, unit, hospital, primary care and community care setting.
Following model development, simulations for various scenarios will be tested, for example, ‘What if intervention A is adopted by 50% of healthcare surgeons?’ or ‘What if patient numbers increase by 10% next year?’ on clinical and economic outcomes.
Using this approach this study aims to adopt implementation science to:
- To identify ways of reducing overuse, underuse and misuse of antibiotics, improving quality of care and reducing waste of healthcare resources
- To promote the efficient design of services by finding solutions along the patient pathway for patients undergoing surgery
- Provide detailed structural, process and behavioural insights of the ‘inner setting’ and ‘characteristics’ of organisational members and patients (constructs of the CFIR framework). An analytical description of existing and potential roles (professionals and patients) along the pathway will be provided.
- Develop provider-patient co-production interventions for sustained effect, variables to measure resource impact of behavioural solutions.
Developing a research programme that includes the above methodologies ensures that the findings and solutions will be driven by stakeholder needs. This approach also considers the balance between intervention fidelity and intervention adaptability. Applying these multi-modal approaches also accounts for the complexity within the phenomena and behaviours under investigation.
Share this
Tackling Antimicrobial Resistance: A Social Science Approach

Tackling Antimicrobial Resistance: A Social Science Approach


Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free







