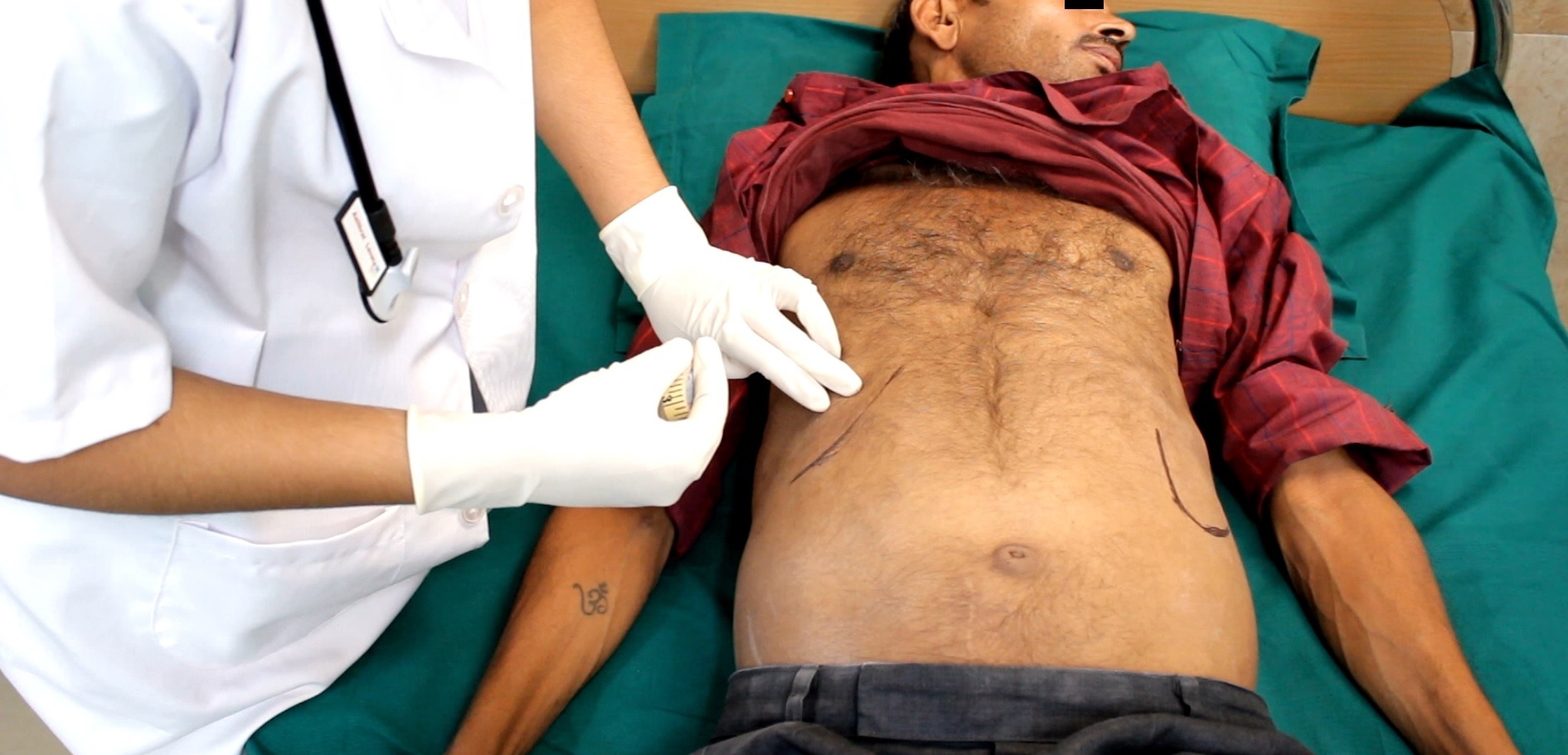
Complex cases of VL and their clinical management – in action
Share this step
In the first run of the MOOC the previous step (2.11) generated a number of learner comments and questions. This supplementary step summarises the issues raised and the response of our course Mentors.
How to treat HIV/VL co-infected patients?
Initiation of VL treatment is an urgent priority in HIV/VL, because the complications of VL disease can be fatal in the short term. Mono-therapy with antileishmanial drugs have shown to be poorly effective (AmBisome, miltefosine) or highly toxic (antimonials) in HIV/VL, and a combination regimen of AmBisome plus miltefosine is recommended. Both drugs are safe, and because of different modes of action effectiveness is enhanced.
Apart from clinical cure, the patient should also be parasitologically cured before discharge. This is because remaining parasites that are not dealt with by the poor immune system of HIV/VL co-infected patients, can lead to rapid relapse. A proportion of patients will need extended treatment with the combination therapy even after a positive test-of-cure.
During VL treatment the patient should be prepared for antiretroviral therapy (ARV or ART, also referred to as HAART), which can start even before finishing VL treatment. Because both VL and HIV suppress CD4+ T-cells, treating both diseases is essential for immune recovery. Patients who are already on HAART when developing VL should continue HAART during VL treatment. Although specific drug-drug interactions between ARVs and anti-leishmanial drugs have hardly been studied, field experience suggests that concurrent treatment is safe.
Notably, Pentamidine, which has been shown to be effective in Ethiopia, cannot be used in the Asian population due to the risk of inducing diabetes. As such, the focus is on identifying a better initial treatment for HIV-VL episodes, and ensuring patients are rapidly started on ART, and screened for TB. These measures alone, if complied with, will make a huge difference in reducing relapses.
Patients with HIV/VL rarely achieve a sterile cure. If these patients, do not adhere to their ART treatment they will always relapse. HIV-VL should be considered a chronic condition for all intents and purposes.
How to manage Malaria/VL co-infected patients?
This was a particular question from one of the learners,
“Malaria infection is endemic in South Sudan, but sometimes outbreaks occur especially in Malaria & VL endemic areas. A pregnant women or child is brought with high fever and convulsion, severe anaemia, enlarged spleen, wasting and RDT test for both Malaria and VL are positive. How will this patient be managed?”
Our clinical mentor has given this response,
“This is a very difficult scenario, where the focus has to be life-saving measures. In this situation, with convulsions, the most critical diagnosis is cerebral malaria. As such, treatment should be initiated for this immediately. If the patient stabilises quickly, then there is time to conduct a splenic biopsy or a bone-marrow aspiration to check for LD bodies. If not, then co-treatment with anti-VL drugs should be initiated (in this case AmBisome would be appropriate). The decision will ultimately lie with the treating physician, but the logic should always be to focus on the riskiest disease first (in this case cerebral malaria). Note that there is some cross-positivity between malaria and rk39 RDT (about 1%), but in areas where both are endemic, one should presume co-infection rather than cross-reactivity.
VL typically does not cause convulsions. However, one must consider febrile convulsions if the child is young (i.e. convulsions due to the fever) or pre-eclampsia in the pregnant woman – therefore, blood pressure should be closely monitored.”
How to treat TB/VL co-infected patients?
To date, there is very limited evidence on the management of TB-VL coinfection and very limited knowledge about drug-drug interactions for VL and TB drugs. One should first ensure that the patient does not also have HIV. Depending on the case and assuming they are HIV negative, then initiating treatment should be as close together as possible. In Asia, there is a tendency to wait for a few days when using MF combination therapies due to the effect on liver transaminases from both MF and ATT therapy, which can result in a rapid transaminitis, requiring stopping of ATT. Generally, in HIV negative patients, VL is the acute illness, and as such, MF can be started for a week and if there is no impact on liver function, ATT can then also be initiated.
How to treat VL during pregnancy?
Treatment of VL during pregnancy must be done very carefully, and ideally only AmBisome used if treatment is deemed necessary. The risks and benefits of clinical management need to be rigorously assessed. Conventional amphotericin B deoxycholate has a high rate of side effects, therefore it needs to be used with care. MF is contraindicated. If the woman is very close to delivery, and the general condition of her pregnancy is good, it is may be worth inducing delivery or waiting for the delivery before initiating treatment unless AmBisome is available. Note that placental transmission of VL has been described in the literature and should be looked out for.
How to manage a patient whilst waiting for a diagnostic result?
Occasionally a patient will have a negative rK39 test but has all the other case-definition symptoms of VL and/or a VL-related history (a suspected relapse case). A confirmatory test such as a Giemsa-stained splenic/bone marrow/lymph node biopsy is instigated but the results may take a while to arrive. Whether VL treatment should be initiated, will depend on the patients’ clinical condition. In 99% of cases, a few extra days of waiting will not make a difference to the clinical outcome, and so symptomatic treatment can be provided while waiting for the parasitological result. In the case of patients who are very unwell and there is high clinical suspicion of VL, the immediate starting of treatment is recommended. Should the biopsy result be negative, it can then be stopped. In such instances, AmBisome should be used, if available, as it is the safest option. AmBisome is indicated in Africa for severely unwell patients.
Share this
Control and Elimination of Visceral Leishmaniasis
Control and Elimination of Visceral Leishmaniasis


Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free







