Occupational health services: Professions and tasks

Share this step
According to ILO Recommendations on Occupational Health Services (No. 171) OHS should be made up of multidisciplinary teams whose composition should be determined by the nature of the duties to be performed. The most common types of professions who work in an OHS are physicians, nurses, physiotherapists, occupational hygienists and safety engineers. In addition they have office staff and some places an OHS can have a psychologist employed or even a priest.
In the literature there is no clear consensus concerning the use of terminology occupational physician / company doctor etc. In this chapter we will use the designation “occupational” health worker (doctor, nurse, hygienist etc.) to indicate that the health worker in question has completed specialized occupational health training.
Occupational physician
The occupational physician, who sometimes is referred to as a company doctor, advises the business on health related and medical issues, and also has the medical responsibility in the OHS unit. In many OHS units the physician is the administrative leader for the OHS. The doctor can participate in health examinations, rehabilitation, supervision and counselling and information work, as well as surveillance of the work places. There are different requirements in different countries to become a competent company doctor/occupational physician, and some countries have a medical specialty in occupational medicine.
Occupational nurse
An occupational, or corporate, nurse works with primary and secondary preventive measures. The nurse can have tasks related to health examinations of workers, counselling and information work, as well as surveillance of the work places. Some countries have specific courses and special education for these nurses.
 An occupational nurse often perform audiometries checking the hearing of the workers. © G. Tjalvin
An occupational nurse often perform audiometries checking the hearing of the workers. © G. Tjalvin
Occupational hygienist
Occupational hygienists are involved in surveillance and supervision related to chemical, biological or physical factors at the work places. Occupational hygienists can have different backgrounds, such as chemistry or biology, and some countries have specialized courses to certify occupational hygienists.
 Occupational hygienists can plan and perform specialized measurements, such as dust measurements, in the work place. © G. Tjalvin
Occupational hygienists can plan and perform specialized measurements, such as dust measurements, in the work place. © G. Tjalvin
Occupational physiotherapist
Occupational physiotherapists work on preventive issues related to musculoskeletal diseases, and often participate in general surveillance and supervision in the work environment. Their main task is to work with prevention of musculoskeletal diseases, but they seldom treat individual persons. Occupational physiotherapists develop their competence by attending different courses, and a few countries have a specialty for this profession related to the work places.
Safety engineer
Some OHS units have their own engineers specialized to work on safety issues at the work places. In some countries the safety engineer and the occupational hygienists have a close co-operation.
General tasks in an OHS
The role of occupational health services should be essentially preventive, and their activity should take into account the particular occupational hazards in the working environment as well as the problems specific to the branches they serve.
The most common tasks that an OHS unit should deal with are in some countries described in the local/national legislation. Otherwise, ILO suggests the following tasks:
a) Surveillance of the working environment
The quality of the working environment through compliance with safety and health standards has to be ensured by surveillance at the workplace. According to The ILO Convention on Occupational Health Services (No. 161), surveillance of the working environment is one of the main tasks of the occupational health services. This can be performed by a walk-through survey of the workplace as well as interviews with managers, foremen and workers. When needed, special safety, hygiene, ergonomic or psychological checks and monitoring can be performed.
b) Informing employer, enterprise management and workers about occupational health hazards
As information about potential workplace health hazards is obtained, it should be communicated to those responsible for implementing preventive and control measures as well as to the workers exposed to these hazards. The information should be as precise and quantitative as possible, describing the preventive measures being taken and explaining what the workers should do to ensure their effectiveness.
c) Assessment of health risks
To assess occupational health risks, information from surveillance of the work environment is combined with information from other sources, such as epidemiological research on particular occupations and exposures, reference values including occupational exposure limits and available statistics. Qualitative (e.g., whether the substance is carcinogenic) and, where possible, quantitative (e.g., what is the degree of exposure) data may demonstrate that workers face health hazards and indicate a need for preventive and control measures.
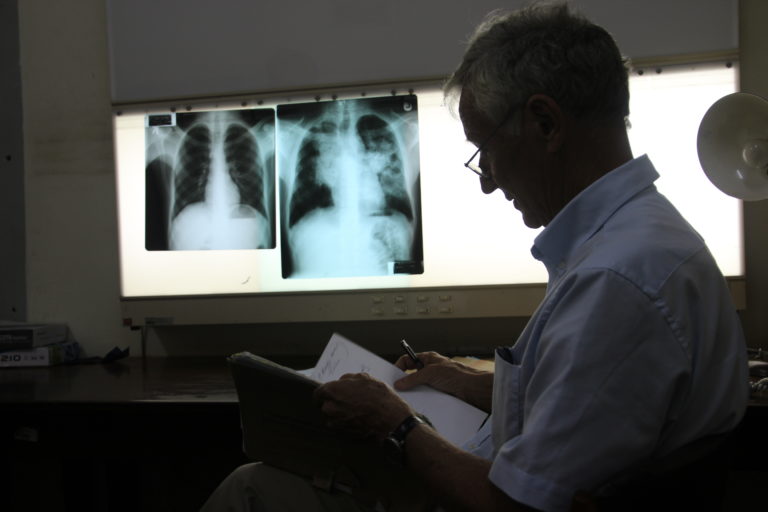 Lung x-rays of a group of workers can be taken, if we suspect development of lung diseases due to a dusty work place. © G. Tjalvin
Lung x-rays of a group of workers can be taken, if we suspect development of lung diseases due to a dusty work place. © G. Tjalvin
d) Surveillance of workers’ health
Due to limitations of a technological and economic nature, it is often not possible to eliminate all health hazards in the workplace. Under such circumstances, surveillance of workers’ health plays a major role. It comprises many forms of medical evaluation of health effects developed as a result of workers’ exposure to occupational health hazards. For instance, if a work place has high noise levels, the hearing ability of the workers can be examined. The purpose is to be able to tell if any of the workers develop reduced hearing. If they do so, they need specific protection and care to avoid further development of the hearing loss, and the work place must work harder on preventive issues to avoid other workers from developing the same problem.
Pre-employment health examinations
Pre-employment health assessment is carried out before the job placement of workers or their assignment to specific tasks which may involve a danger to their own health or that of others. The purpose of this health assessment is to determine whether a person is physically and psychologically fit to perform a particular job and to ensure that his or her placement in this job will not represent a danger to his or her health or to the health of other workers. This work is not always a task for an OHS unit. Pre-employment examinations might put the occupational physician into a difficult position. These examinations require that an evaluation is made; to find out if the worker fits in or not. This is another role than the one a physician in an OHS normally has; being a support for the worker. The physician who performs pre-employment examinations must think this through and know what kind of role he/she is assuming.
e) Advisory role in decision-making processes
An important task for occupational health services is to provide advice to the enterprise management, the employers, the workers, and health and safety committees in their collective as well as individual capacities. Such advice needs to be taken into account in any company decision-making processes, especially if the occupational health professionals are not directly involved in the decision-making.
f) Occupational health care and curative health services
Occupational health services may be involved in the diagnosis, treatment and rehabilitation of occupational injuries and diseases. The knowledge of occupational diseases and injuries combined with the knowledge of the job, the working environment and occupational exposures present in the workplace enable the occupational health professionals to play a key role in the management of work-related health problems. General curative health services are not normally recommended as a part of the OHS activity, as this work may steal time from the preventive issues. However, in low income countries the situation might be different. In low income countries, health services in general might be lacking, and employees will need these services. For an OHS to be able to treat a worker with malaria might be extremely useful if the alternative is no treatment at all. However, when curative work and ordinary OHS work is mixed, the OHS personnel should be very aware of the difference in tasks and not end up only undertaking curative activities. The prevention is after all the main aim of an OHS.
g) Rehabilitation
The participation of occupational health services is particularly crucial in guiding workers’ rehabilitation and their return to work. This is becoming more and more important as there are a large number of occupational accidents in developing countries and in terms of the ageing of the working populations in industrialized societies. OHS may play an important role in seeing that workers recovering from injury or disease are referred to them promptly. It has been shown to be preferable, when practicable, for a worker to return to his or her original place of employment. It is an important function of OHS to maintain contact during the period of incapacity with those responsible for treatment during the acute stages in order to identify the time when a return to work can be envisaged.
h) Health promotion activities
 Many occupational health services participate in “stop smoking” campaigns. © G. Tjalvin
Many occupational health services participate in “stop smoking” campaigns. © G. Tjalvin
There is some tendency, particularly in North America and Europe, to incorporate wellness promotion activities in the form of occupational health programs. These programs are, however, essentially general health promotion programs that may include such elements as health education, stress management and assessment of health risks. They usually aim at changing personal health practices such as alcohol and drug abuse, smoking, diet and physical exercise, with a view to improving overall health status and reducing absenteeism. These programs, designed as health promotion programs, though valuable as such, are not usually considered as occupational health programs, but as public health services delivered in the workplace, because they focus attention and resources on personal health habits rather than on protection of workers against occupational hazards.
Share this
Occupational Health in Developing Countries

Occupational Health in Developing Countries


Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free







