Home / Healthcare & Medicine / Antimicrobial & Antibiotic Resistance / COVID-19: Global Health Perspectives / Ebola Lessons For COVID-19 Response

Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.

 Sierra Leone: Tracing Ebola in Tonkolili. Source:
Sierra Leone: Tracing Ebola in Tonkolili. Source: 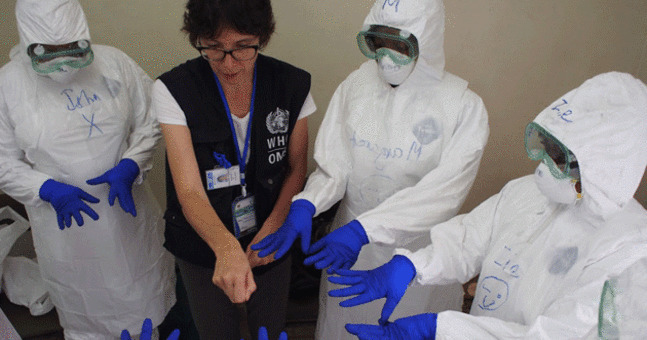 Multidisciplinary teams deployed to the field to detect and manage cases and trace their contacts. Source:
Multidisciplinary teams deployed to the field to detect and manage cases and trace their contacts. Source:  Maintaining continuation and safety of medical services in Guinea. Source:
Maintaining continuation and safety of medical services in Guinea. Source:  Successful Ebola responses in Nigeria, Senegal and Mali. Source:
Successful Ebola responses in Nigeria, Senegal and Mali. Source: 






