Recording Pathological Bone

The specific cause of abnormal bone cannot always be identified. Careful descriptive analysis is therefore of key importance. The renowned expert in skeletal pathology Don Ortner identified three essential elements for recording skeletal pathology:
- A clear and unambiguous terminology to describe pathological changes
- Identify precisely the location and distribution of the abnormal bone
- Provide a clear descriptive summary of the morphology of the abnormal bone
Recording Pathological Lesions
First and foremost, it is important to record the location of the pathological lesion (identify the bone and where on the bone- anterior/posterior, proximal/distal). To make your description both detailed and clear, it can be useful to record pathological lesions on bone by addressing a series of questions. Some particularly helpful examples are provided below.
- Does the lesion have multiple foci, or a single?
- Is it localized (affecting just one area of the bone) or diffuse (spread across a large area of the bone)?
- Is it bone destruction, or bone growth (or both)?
- Is the lesion active (e.g. woven bone present), or healing/healed (remodeled edges)?
- What is the morphology of the lesion (is it pitted, or striated, is it irregular)? Provide a description.
- Is only one bone affected or are a number of bones across the skeleton affected? If the latter, then show this on a skeletal chart.
- What is the extent of the lesion (e.g. does it involve the periosteum- the outer bone surface, the cortex, or medullary cavity)?
- What is the size of the lesion?
- What are the margins of the lesion like?
- Does it appear to be secondary to another disease process (e.g. a poorly healed fracture might lead to joint disease)?
- Is there evidence of deformity in the bone’s normal morphology?
 Both of these femora are from non-adults of similar ages. The top femur is normal and the bottom femur is displaying the bowing typically associated with vitamin D deficiency, or rickets.
Both of these femora are from non-adults of similar ages. The top femur is normal and the bottom femur is displaying the bowing typically associated with vitamin D deficiency, or rickets.
Pseudopathology
When a body is buried there are numerous forces acting on it in the burial environment, from animals, insects, plants, and bacteria to chemical exchanges with the groundwater. Post-mortem changes in human bone can resemble pathological changes and it is important not to confuse them.
These include:
- Root or other damage by adjacent plants
- Gnawing by rodents or other animals (teeth marks by rodents can be mistaken for cutmarks)
- Chemical weathering (acids in the soils can etch the bones in ways that can look pathological)
- The action of fungi or moulds
- Staining of the bones from objects associated with the body (e.g. metals)
In addition, there is a variety of normal skeletal features that vary slightly from person to person. A less experienced osteologist may mistake some of these features for pathologies rather than normal variation. These are referred to as non-metric traits.
Commonly confused traits include:
- Arachnoid depressions, which are normal pits on the inner surface of the cranial vault
- Parietal foramina (holes in the parietal bones of the skull which can sometimes be quite large)
- Sternal foramen (hole in the sternum, which is not pathological)
- Developmental defects in the talus (can be confused with a condition called osteochondritis dissecans)
Some individuals are much more robust (large and muscular) than others and this will affect the morphology of the bones to a degree. Students often confuse a very robust deltoid tuberosity (the muscle attachment site for the deltoid on the shaft of the humerus) for a healed fracture as it appears to deform the humeral shaft.
Another key source of confusion relates to the bones of infant and children. Bones which are still growing and developing are formed of several distinct parts until maturity, when fusion occurs. This process should not be confused with fractures or other forms pathology. Further, childhood is a period of very rapid growth. The normal new bone that is forming can look very similar to woven bone produced in response to pathology. It is useful therefore to exercise particular caution when diagnosing pathology in younger individuals.
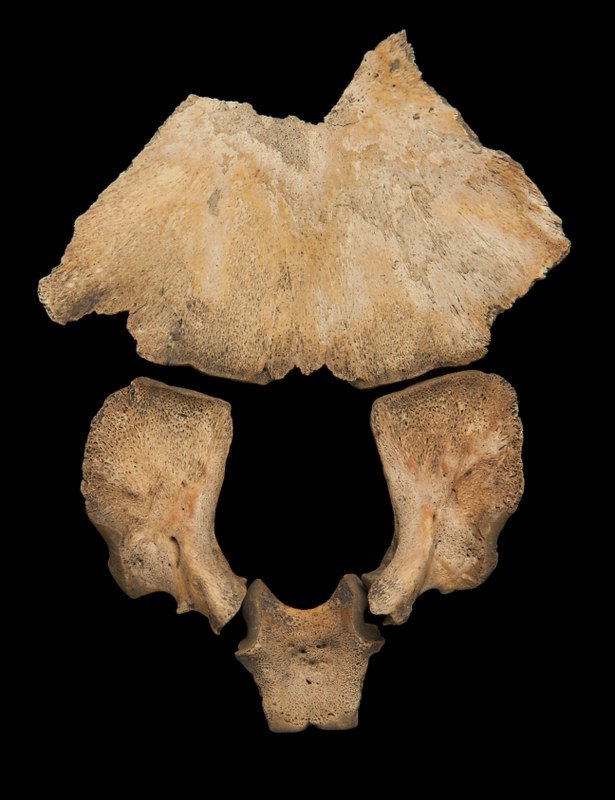 A non-adult occipital bone showing the pars basilaris, pars lateralis and squamous section before fusion. This is normal development and not pathological.
A non-adult occipital bone showing the pars basilaris, pars lateralis and squamous section before fusion. This is normal development and not pathological.
Differential Diagnosis
Bone has a limited response to a wide variety of pathological conditions. As a result, it is not always possible to diagnose a condition. Sometimes there can be several possible causes for an observed skeletal abnormality. All of these should be stated and discussed, with the most likely cause emphasised.
Limitations to Recording and Interpreting Skeletal Pathology
Preservation
Sometimes skeletons are badly damaged by factors acting on the body in the ground, which can cause the bones to become very fragmented, or completed destroyed. Sometimes the skeleton is complete, but the outer surface of the bone has been eroded. All of these factors make it harder (and sometimes impossible) to identify, record and diagnose pathological conditions.
Not all diseases will affect the skeleton
If we think about the many infectious diseases that we have had throughout our lives, most are short-lived (e.g. chickenpox, or flu). These will not affect our bones. Only longer-term, chronic conditions will affect the skeleton and usually only in the absence of treatment. A variety of other pathological conditions will, however, be observable on the bones. For example, congenital conditions (e.g. hip dysplasia), joint disease, metabolic disease (e.g. vitamin D deficiency), some forms of cancer, and hormonal imbalances may still be visible.
People respond differently to diseases
Everyone is different and this includes our immune response, or our ability to respond to conditions such as joint disease. As a result, the same disease can affect the bones of people differently and this can create challenges.
Infants and children
Young individuals with immature immune systems may die before the disease affects their skeleton. On the other hand, their growing skeletons can be very sensitive to adverse living environments or poor diet and they can show a variety of skeletal indicators that reflect these poor conditions.
Recording pathological lesions requires practice. Try out your recording skills with the 3D models provided in the ‘SEE ALSO’ section below. Then practice recording and coming up with a differential diagnosis in the following discussion.
Share this

Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free








