Pregnant women and exposure in developing countries

Share this step
While there is an overall lack of knowledge, there are a number of workplace hazards that have been identified as being linked to reproductive health problems. In this article, we will tell you more about some of these, and give you some examples of occupations that are particularly at risk. We will give you some tips on how to manage pregnant workers who are exposed to different hazards. However, it is important to remember that the management of pregnant workers is often difficult because, in many occupations, pregnant women are exposed to several risk factors. Because of potentially devastating results, we underline again that the principle of “better safe than sorry”, should be used in the management of pregnant workers.
Risk assessment
The principles and process of risk assessment were described in more detail during the first week of this course. Here we will only remind you that risk assessments must be based upon to two elements: identification of the hazards and assessment of the exposure levels for the people at risk.
Health effects
Health effects related to reproductive health includes all states where the fetus does not develop normally; miscarriage, premature birth, growth retardation in the fetus, stillbirth and congenital malformations. Health effects due to exposure during fetal life may also manifest themselves later in life.
Different aspects of exposure can affect the outcome during all the reproductive phases:
Before conception:
- Exposure leading to decreased fertility of the mother or father.
Different kinds of exposure can reduce the fertility in both men and women, resulting in no conception. © Colourbox
- Exposure that give live babies with structural malformations, functional changes, diseases and prematurity complications.
- Exposure that give stillborn babies with structural malformations, functional changes, and complications of abortion or premature birth.
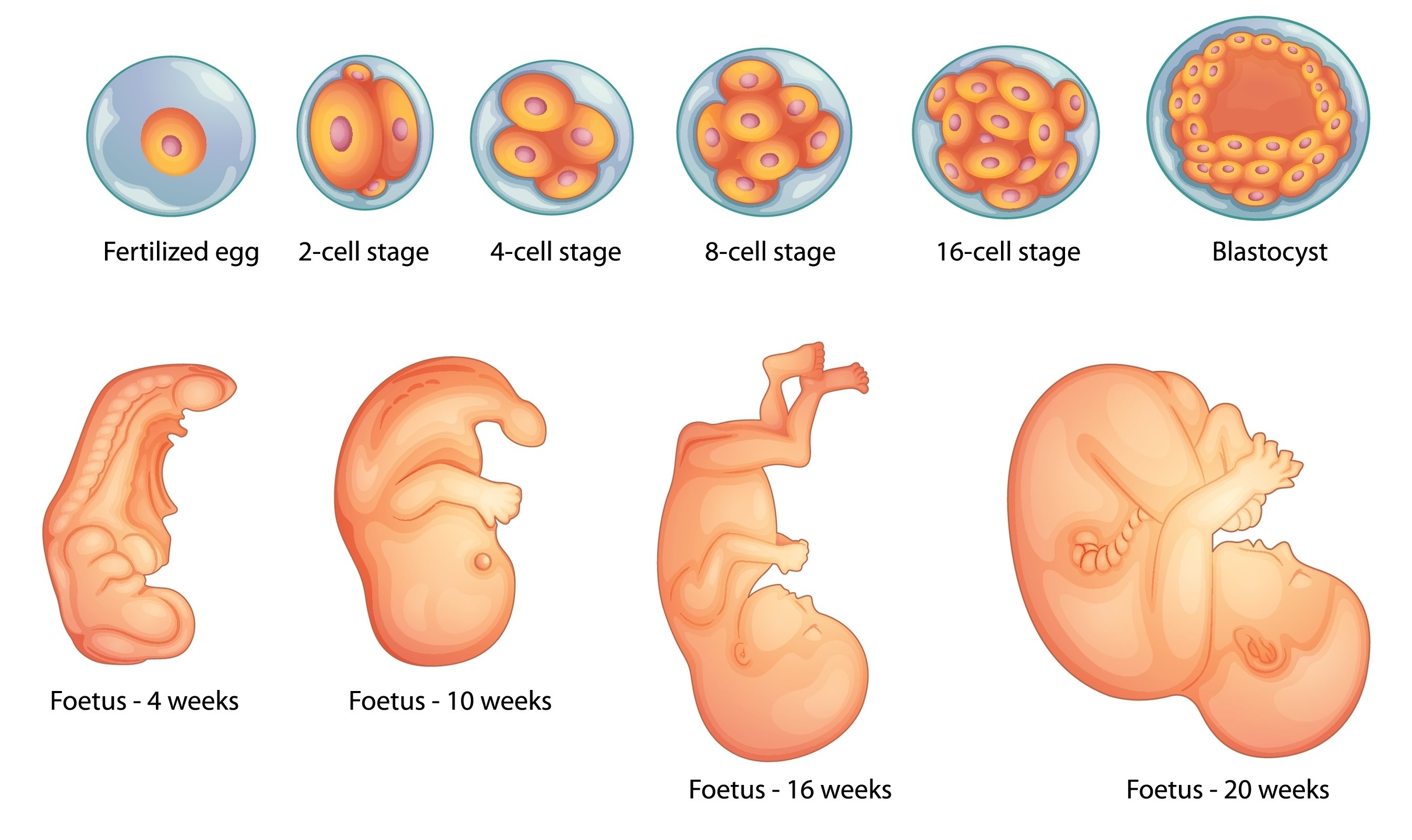 The developing fetus is most vulnerable to toxic chemicals during the first eight weeks of pregnancy and potentially before the woman knows she is pregnant. Other factors could be most harmful during other phases of the pregnancy. © Colourbox
The developing fetus is most vulnerable to toxic chemicals during the first eight weeks of pregnancy and potentially before the woman knows she is pregnant. Other factors could be most harmful during other phases of the pregnancy. © Colourbox
- Exposure through breastfeeding causing disease in the child.

Most mothers who work can safely breastfeed their babies. Some chemicals have, however, been measured in breast milk at levels that could harm the baby. Examples include heavy metals such as lead and mercury, organic solvents and some radioactive chemicals. © Colourbox
Exposure factors
Chemical hazards
Before we start telling you about chemical hazards, we will present some basic concepts and definitions:
Reprotoxic substances (substances toxic to reproduction):
Reprotoxic substances are agents that cause adverse effects on sexual function and fertility in females and males, and that have developmental toxicity in the offspring. Effects that are transmissible via lactation to breastfed babies are also included in this group.
Mutagen:
The term refers to agents that cause an adverse effect on a person’s genetic material. Mutagens include substances or agents that are capable of causing a permanent change in the amount or structure of the genetic material in a cell.
Carcinogen:
Carcinogens are substances or mixtures that induce cancer/uncontrolled growth of altered cells. Carcinogenic, mutagenic and reprotoxic substances are often referred to as a group, because a substance may have all three effects. They are grouped together because of similarities in their classification and also in terms of legislation. The abbreviation “CMR” is commonly used to label this group, for instance, in safety data sheets (SDSs).
Teratogen:
The term teratogen refers to an adverse effect on the fetus. Substances or agents that can interfere with normal embryonic development and cause malformations or defects to an embryo or fetus are called teratogens.
When a pregnant women is exposed to toxic chemicals, the fetus will usually also be exposed, via the placenta. The developing fetus is most vulnerable to toxic chemicals during the first eight weeks of pregnancy and potentially before the woman knows that she is pregnant. Because the fetal liver has a limited capacity to detoxify harmful chemicals, fetuses are particularly vulnerable to the effects of toxic chemicals, and exposure to such agents could result in birth defects or even spontaneous abortion.
Pregnant women should not handle carcinogenic, mutagenic or reprotoxic (“CMR”) substances before a risk assessment has been carried out, and actions taken accordingly, to minimize exposure.
Pregnant women are at risk of being exposed to “CMR”-substances in many different occupations. Examples include laboratory assistants, health care personnel or pharmacists handling chemotherapeutic drugs as well as workers in a wide range of chemical process industries.
Laboratory assistants potentially handle many different chemicals that are classified as “CMR”-substances. © G. Tjalvin
Farmers and employees in the floriculture industry are also at high risk as many pesticides are classified as “CMR”-substances.
Many pesticides are fat-soluble and can accumulate in the body’s fat-tissues. © Colourbox
Exposure to organic solvents is considered harmful for pregnant women at levels far below accepted occupational exposure limits, even though many of them are not classified as “CMR”-substances. However, some organic solvents are classified as teratogens. Also some heavy metals, such as lead and mercury are classified as teratogens, and hence pregnant women should avoid exposure to these.
Workers employed in the paint industry are exposed to different organic solvents. Such exposure is considered harmful to pregnant women at levels far below accepted occupational exposure limits. In some studies a positive association has been observed between maternal exposure as a painter (including pre-conception and during pregnancy) and childhood leukemia in the child. © G. Tjalvin
Biological hazards
Biological agents, such as different viruses and bacteria, can impair fertility and can also be passed from the pregnant woman, via the placenta, to the fetus with devastating effects. If the mother has not acquired immunity, several infections during pregnancy, including rubella, chicken pox, hepatitis B and toxoplasmosis have been linked with birth defects and miscarriages. Health care personnel, laboratory assistants, kindergarten assistants and teachers are at the greatest risk for such biological hazards.
Rubella
Rubella is generally a mild, self-limited disease associated with a characteristic exanthema, and many cases the illness is subclinical or asymptomatic, especially among young children. Maternal immunity, either via vaccine or naturally derived, is protective against intrauterine rubella infection, but the proportion of rubella-susceptible women of childbearing age varies greatly between countries, especially in developing countries. In Nigeria, 23 % of women of childbearing age had negative titers. The most frequent defect associated with congenital rubella syndrome is hearing loss, followed by mental retardation, cardiovascular defects, and ocular defects. The risk of congenital defects after maternal infection is essentially limited to maternal infection in the first 16 weeks of pregnancy.
Teachers are at risk of being infected by different viruses that could harm a developing fetus. © G. Tjalvin
Toxoplasmosis
Work that includes contact with certain types of animals or meat can lead to infection with toxoplasmosis in the pregnant woman. The Toxoplasma parasite (the oocyst form) is shed in cat feces and becomes infective one to five days later. It may remain infectious for over a year, especially in warm, humid environments. Humans who come in contact with cat feces containing Toxoplasma oocysts may inadvertently ingest contaminated material. Food animals such as pigs, chickens, lambs and goats become infected by the same routes as humans, resulting in meat that contains tissue cysts (the infectious form of the parasite). Hence, workers in occupations that include the handling of raw meat are at risk of becoming infected.
The Toxoplasma parasite is mainly acquired during childhood and adolescence. In industrially developed, temperate climate countries, 10-50 % of adults aged 15-45 years display serological evidence of past infection. Much higher rates of past infection, up to 80 %, are found in the tropics in communities exposed to contaminated soil, undercooked meat, or unfiltered water. When a toxoplasma infection is acquired for the first time during pregnancy, infection can be transmitted to the fetus, resulting in congenital toxoplasmosis. As the gestational age increases, the risk of infection in the fetus increases, but the severity of the disease decreases. Congenital toxoplasmosis is associated with fetal death and abortion. In infants, it is associated with neurologic deficits and neurocognitive deficits.

Contact with feces from cats can lead to infection with toxoplasmosis. If a woman is infected for the first time during pregnancy, it can have devastating effects on the fetus. © G. Tjalvin
Physical hazards
Ionizing radiation
Ionizing radiation is known to have damaging effects on fertility in both women and men. In the developing embryo/fetus exposure to ionizing radiation can be teratogenic, carcinogenic, or mutagenic. The effects are directly related to the level of exposure and stage of fetal development. The fetus is most susceptible to radiation during organogenesis (2-7 weeks after conception) and in the early fetal period (8-15 weeks after conception). Spontaneous abortion, growth restriction, and mental retardation may occur at higher exposure levels. The risk of childhood malignancy, especially leukemia, is increased regardless of the dose.
Radiologists and others who work with radioactive materials are at risk of being exposed to radiation doses at levels that could be harmful for the unborn child. Care should be taken to keep doses as low as possible and within acceptable limits. Rules for radiation dose limits apply once a pregnant employee declares her pregnancy.
Ionizing radiation is known to have damaging effects on the fertility of both women and men, as well as on a developing fetus. In-utero exposure to X-radiation can cause childhood cancer. © G. Tjalvin
Whole body vibration
Whole body vibration is another physical agent that has been associated with miscarriages, growth restrictions, fetal death and premature deliveries. Pregnant women should therefore avoid high levels of vibration and/or prolonged exposure. Low frequencies seem to be most harmful, and the exposure is most dangerous to the fetus during the first and the last trimester.
More men than women are exposed to whole body vibration because typical occupations at risk, such as helicopter pilots and machine operators, are typically dominated by male workers.
Noise
Many pregnant women are exposed to noise at the workplace. This is true for employees in a number of different kinds of industry. Prolonged exposure to loud noise can lead to increased blood pressure and tiredness in the mother. The human cochlea and peripheral sensory end organs complete their normal development by 24 weeks of gestation. During the rest of the pregnancy, excessive noise may also result in high-frequency hearing loss in newborns. Exposure to noise during pregnancy has even been associated with prematurity and intrauterine growth retardation, but the knowledge about these effects is limited.
In terms of managing a pregnant worker exposed to excessive noise, it should be noted that the mother’s use of personal protective equipment will not protect the unborn child from the hazard. Rather, the fact that the pregnant woman must wear hearing protection is an indication of a harmful work environment for the fetus. Noise with a low frequency (<500Hz) is more harmful to the fetus than noise with a high frequency.
Hearing protection worn by the mother will not protect the unborn child from the hazard of noise exposure. © G. Tjalvin
Extreme heat
Heat stress can also be a problem for pregnant women as they are less tolerant to heat. During pregnancy the blood vessels dilate and hence the blood pressure drops. After birth, heat exposure can also lead to dehydration, which may impair breast-feeding. Exposure to high temperatures at the workplace can also cause reduced fertility among men.

Exposure to high temperatures at the workplace can cause reduced fertility among men. © G. Tjalvin
Ergonomic factors
Pregnant women undergo physiological changes during pregnancy. Hormonal changes can increase muscle tension and cause ligament softening. As the pregnancy progresses, jobs that involve heavy lifting and standing for most of the working day combined with the body changes due to pregnancy increase pregnant women’s risk of developing musculoskeletal diseases. Physically demanding work is also suspected as causing growth retardation in the fetus and preterm birth, but the knowledge of this effect is limited.

Many women carry heavy weight during their working day. Knowledge about this potential hazard is limited, but it is believed that physically demanding work might cause preterm labour. © G. Tjalvin
Workplaces and processes should be ergonomically evaluated to reduce risks for pregnant women. Where possible, lifting aids should be used to avoid the need for pregnant workers to lift heavy weights, and work stations and processes should be ergonomically designed to avoid repetitive movements, static postures over long periods, and tasks that include twisting or stretching. When performing risk assessments it is important to consider the physical changes that a pregnant worker will undergo during the course of the pregnancy and keep in mind that it might be necessary to make a series of modifications at various stages of the pregnancy.
The health care sector is characterized both by physically demanding work and standing or walking most of the working hours. Hairdressers are also standing for most of their working hours and are at the same time exposed to a variety of chemicals.

In many occupations, pregnant women are exposed to several risk factors. Hairdressers, for instance, are exposed to a variety of chemicals, and are standing for most of their working hours. © G. Tjalvin
Psychosocial factors and stress
Pregnancy can compromise the work capacity of the pregnant worker and cause stress. Long working hours and a heavy workload have been linked with an increased risk of preterm birth and low birth weights. High blood pressure can decrease blood flow to the placenta and might lead to preterm labour, low birth weights and even pre-eclampsia, which, if untreated, can lead to serious and potentially fatal complications for both the mother and the baby. Stress has also been shown to increase the risk of post-natal depression.
Share this
Occupational Health in Developing Countries

Occupational Health in Developing Countries


Reach your personal and professional goals
Unlock access to hundreds of expert online courses and degrees from top universities and educators to gain accredited qualifications and professional CV-building certificates.
Join over 18 million learners to launch, switch or build upon your career, all at your own pace, across a wide range of topic areas.
Register to receive updates
-
Create an account to receive our newsletter, course recommendations and promotions.
Register for free







